What I want to look at in this piece is the way politicians and the media are talking about risk in relation to the lockdown. We are constantly being told of the risk that covid poses and the need for more lockdown. What is often sidelined or ignored completely is the risk that a lockdown poses in itself.
Let’s start with Keir Starmer’s press conference yesterday:
The number of Covid cases has quadrupled in the last three weeks. Cases may be doubling as quickly as every seven to eight days. There are now more people in hospital with Covid than on 23 March when we went into national lockdown. And while the number of cases is rising more sharply in some areas it is increasing across all regions of the UK and in all age groups.
We know from bitter experience and great personal loss where all this leads. Three things are now clear: the Government has not got a credible plan to slow infections. It has lost control of the virus. And it’s no longer following the scientific advice.
The SAGE minutes from 21 September – published yesterday – underline this. They warn that: ‘A package’ of ‘stringent interventions’ is now urgently needed. SAGE also says that: ‘not acting now… will result in a very large epidemic with catastrophic consequences.’
Focussing on what might happen
The first thing I notice is that the focus is based on predictions of what is going to happen in the future. He says “we know … where all this leads”. If we don’t act now, according to SAGE, it will result in a “very large epidemic with catastrophic consequences”. It’s as if his prediction of the future is a foregone conclusion.
This is the kind of language I see all the time. It’s the primary reason why many people are against a herd immunity strategy. For example, as this New Scientist blog published today says, “We don’t yet know whether natural immunity to SARS-CoV-2 (or the experimental vaccines) will halt transmission. Until we do, assuming that herd immunity will automatically appear is unscientific and, frankly, irresponsible.”
So a herd immunity strategy is “irresponsible”, because we don’t know if it will happen or not. We don’t know – so let’s play it on the safe side. Let’s be safe and not take the risk. This is the message which we are hearing all the time from the government, from scientists, from the media. “Better safe than sorry”.
The problem with ‘better safe than sorry’
I think “better safe than sorry” is generally good advice. But, like a lot of good advice, you can go too far with it. There’s a funny scene at the start of the film Ratatouille.
An old lady spots a rat, and so she decides to deal with it in a perfectly proportionate way… with a shotgun. She ends up basically destroying her house! The action she took ended up doing far more damage than the danger.
You could think of many other examples. If you take the principle to its logical conclusion, you’d never do anything risky. In fact, you’d probably never leave the house – but wait, staying in the house carries an element of risk! And that’s the point: being alive carries an element of risk with it. We can mitigate against some risks, but there has to come a point at which we say “well, that’s a risk we’re just going to have to take”.
I know that driving is risky, for example. But I weigh up the risks and, in general, decide that the risks are pretty low and that it’s of more value to me personally to get somewhere quickly. Everyone has to accept a measure of risk in everything, but in general most of us don’t think about the risks too much. And we survive!
There’s more than one kind of risk
Add to that the fact that risk applies in more than one way. Let’s go back to the example of driving. Driving a car carries a risk. But then, what if I decide to walk? Walking carries a risk too – in fact there might be a greater risk of being run over. If I decide to cycle, again – there are risks involved. But think about it more deeply: if I drive everywhere, maybe I’ll become obese. Maybe I’ll die early of heart disease. Cycling or walking may be a bit more risky, but I’ll get more healthy.
The point is that there are risks in every area of life – no matter which course of action we take. We have to balance those risks every day. Most of us are pretty good at it – we decide what level of risk is appropriate for us, and we act accordingly. But the point is that we all have to balance risk no matter what we do.
So this brings us onto the question of the lockdown. In the speech I quoted at the start, Keir Starmer said a ‘circuit breaker’ lockdown would avert one risk – of people dying from covid. However, what he didn’t say is that there will be risks of another lockdown. I think we should consider those risks.
Also – just to re-iterate: the risks of not locking down are a “maybe”. We’ll think a little about the actual chances of that happening below. But we can see the risks of lockdowns right now.
Risks of another lockdown
The Economy
The UK has plunged into the largest recession on record since the start of the lockdown. There could be over 700,000 redundancies in the autumn alone – bringing the total for 2020 to over one million. I don’t know anyone personally who has died of covid – I do know several people who have either lost jobs or face extreme uncertainty about whether they’ll be going back to jobs.
And we should say that a strong economy has health benefits: where does the money for the NHS come from? From the taxpayer. If the government are spending more money for people who are unemployed, and collecting less tax, the NHS is going to suffer. A recession is not going to help public health.
Health in other areas
The lockdown has meant that many people who would (and should) have been treated for other conditions have been staying away from hospital. For example, Prof Karol Sikora warned that cancer was the next big crisis facing the NHS, because of the number of people who had not received a diagnosis. The Sun reported that hundreds of stroke and heart attacks have gone untreated.
This is what a registered nurse had to say:
The hospital had speciality wards for medical emergencies such as strokes, which were always full (before Covid). An emergency episode like a stroke can be easily diagnosed and treated with thrombolytic therapy, a hugely vital service preventing death and worsening brain injuries. The stroke ward was virtually empty. … It makes me shudder to think that these people, mainly the elderly again, collapsed and likely died at home as coming into hospital for treatment no longer seemed an option for them.
I nursed a 50-year-old lady last week who was diagnosed in January with aggressive breast cancer. Her mastectomy was planned for early March but was then cancelled. She had no contact with the Oncology Team and only just had her mastectomy 3 weeks ago. When I met her, she was waiting on the results of her recent MRI to see if her cancer had spread anywhere else. She has really experienced a lot of fear this year.
I have heard anecdotally from people I’ve spoken to that these experiences are not uncommon. Someone I know from the school gate says a friend has been delayed treatment due to covid. People are being discouraged from visiting GPs. I’ve read reports of nearly-empty GP surgeries. Where are all the people who would normally be there? Surely illnesses are not simply going away?
Mental Health
I think mental health is quite possibly the biggest risk which is not being talked about. I think there is a massive issue bubbling away under the surface. The ONS, for example, reported on 9th October:
Average anxiety scores for adults have increased to their highest level since April at 4.3 this week, according to the latest Opinions and Lifestyle Survey (OPN).
Of those who reported that their wellbeing has been affected by the coronavirus pandemic, 63% said they felt stressed or anxious, while 64% said they felt worried about the future.
Over 60% of people are feeling stressed and anxious. Now that’s an epidemic – a mental health epidemic. Similarly, ONS data from June says:
Almost one in five adults (19.2%) were likely to be experiencing some form of depression during the coronavirus (COVID-19) pandemic in June 2020; this had almost doubled from around 1 in 10 (9.7%) before the pandemic (July 2019 to March 2020).
One in eight adults (12.9%) developed moderate to severe depressive symptoms during the pandemic, while a further 6.2% of the population continued to experience this level of depressive symptoms; around 1 in 25 adults (3.5%) saw an improvement over this period.
Many British people right now are feeling anxious and depressed. I can testify to this from my own experience! But I’m particularly worried about the effect this is having on a younger generation. For example, one of my wife’s co-workers said her daughter’s class (primary school age) are all really anxious at the moment. Someone at church said before the summer, her granddaughter refused to go back to school when she had the opportunity (she was in year six) because she was so terrified.
The lockdown directly impacts our mental health. I know of several people who are really struggling at the moment. Another lockdown would compound the mental health problem. We shouldn’t be surprised about this given that a lockdown essentially prevents us from doing what human beings are supposed to do.
Is the risk worth it?
This is the million dollar question, so to speak. I wouldn’t like to be a politician at the moment, to have to balance these kind of things. Personally, I don’t think the risk of another lockdown is worth the benefit of maybe saving lives. I say maybe because, as I said at the start, the ‘circuit breaker’ lockdown is based on a prediction of the future. This is a complicated subject, and it’s one I’m not a specialist in. But I think there are a few reasons to be optimistic.
The death rate is nothing like it was at the peak
This graph shows the number of weekly deaths which name covid on the death certificate. As you can see, it climbs very sharply at the beginning of April, and then in the middle of April things begin to fall off again. As you can see on the graph, deaths are beginning to climb a little but it’s nothing like what we saw in April. There’s a similar picture in other countries, too, such as France and Spain.
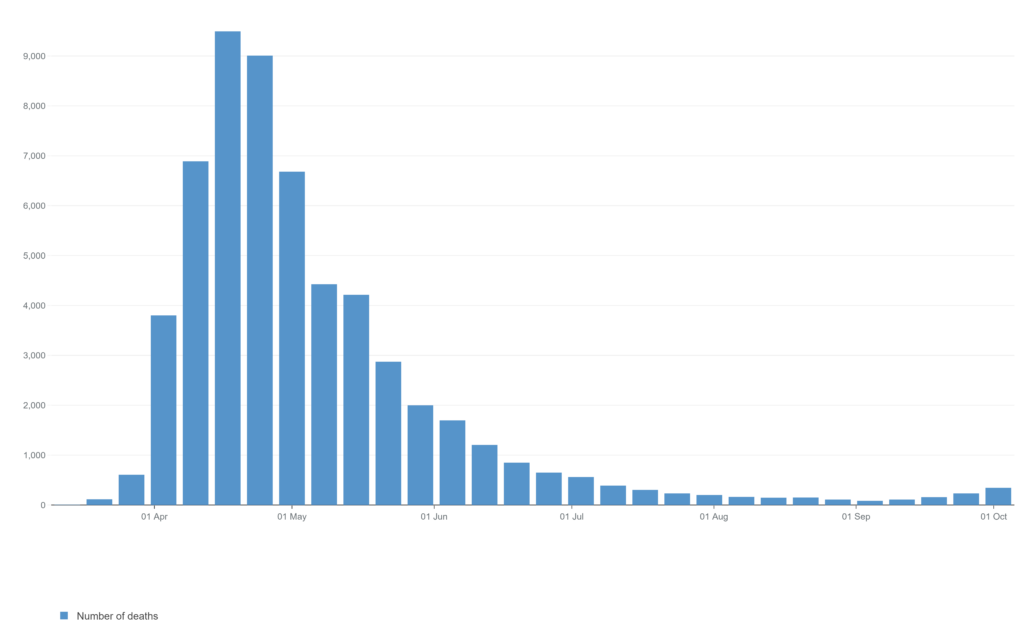
In fact, some people say that the peak actually happened before the full lockdown restrictions were introduced (if you take into account the typical time between infection and death).
Lockdowns don’t work
Recently the WHO Covid-19 envoy David Nabarro said they did not recommend lockdowns apart from a short measure to ease pressure on health services. Some scientists are now saying that there is little to no evidence that lockdowns actually work:
In a National Bureau of Economic Research paper published last month, UCLA economist Andrew Atkeson and two other researchers, after looking at COVID-19 trends in 23 countries and 25 U.S. states that had seen more than 1,000 deaths from the disease by late July, found little evidence that variations in policy explain the course of the epidemic in different places.
There are other voices saying the same thing. There’s very little correlation between the way a country has responded to the virus and the number of deaths.
Even in the UK, there is some doubt as to whether local lockdowns have done anything to actually slow the spread of the virus.
There are many other angles we could talk about here, such as the fact that the average age of death from covid is about 82 (average life expectancy in the UK is about 82). We could go on – but let’s leave it there.
Let’s wrap this up
One of the problems with a lockdown is that it’s a blunt instrument. It’s like using a sledgehammer to crack a nut: you might crack the nut, but you might break a few other things in the process. My feeling is that many of our politicians and the media are keen to use the sledgehammer of lockdown without considering the risks of that strategy. I think this is doubly the case given that it’s unclear how much benefit lockdowns actually bring. Is it actually possible to control the virus?
Would a better strategy be something such as what the Great Barrington Declaration says? I’ll leave you to make your own mind up.

Leave a Reply